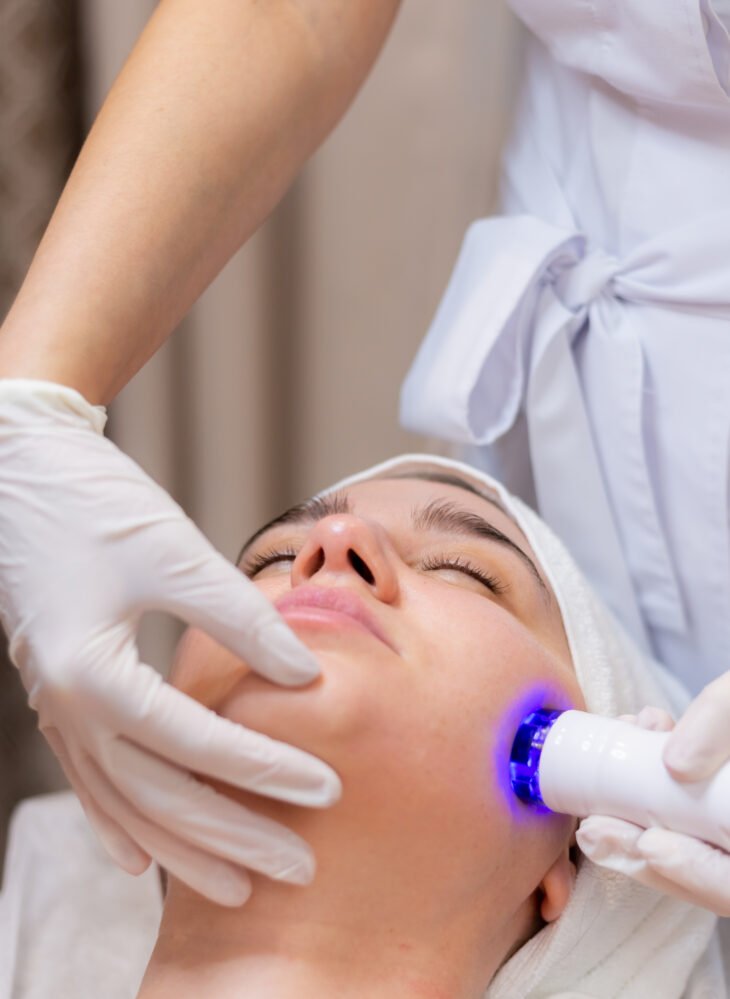
Aesthetic procedures—from injectables and lasers to surgery—continue to rise globally, and professional societies such as ISAPS and ASPS have consistently reported year‑over‑year growth across both surgical and non‑surgical categories. What many first‑time international patients don’t realise is that outcomes are shaped not only by what happens in the treatment room, but by what you do before and after—your screening, preparation, downtime planning, and adherence to aftercare instructions. If you’re considering treatment abroad, the goal is not to rush decisions; it’s to reduce risk with clear steps, verified providers, and realistic recovery planning.
This guide is educational and can’t replace your clinician’s personalised instructions—protocols vary by patient and provider—yet it will help you understand the process and recognise time‑sensitive red flags (for example, vascular compromise after fillers and clot symptoms after surgery require urgent assessment).
This article walks you through a universal before‑care framework, a universal aftercare framework, procedure‑specific playbooks, downtime planning, myth‑busting, and clear red‑flag guidance.
Why aftercare for aesthetic procedures is part of the procedure, not an optional add‑on
Aftercare doesn’t begin at discharge. It starts at screening and provider verification—because many complications are influenced by candidate selection, facility standards, and whether patients follow instructions closely.
Common issues seen across aesthetic procedures include:
- Infection (from minor to serious)
- Poor wound healing and delayed recovery
- Scarring or texture changes
- Pigment changes, including post‑inflammatory hyperpigmentation (PIH)
- Prolonged swelling and bruising
- Vascular compromise (injectables—time‑critical)
- Thromboembolism risk after surgery (time‑critical)
A key safety layer is ensuring the practitioner is appropriately trained and the setting follows robust infection prevention practices. The CDC’s infection control guidance underscores how infections spread in healthcare environments and why standard precautions and hand hygiene matter in every clinical setting (including aesthetic clinics).
External reference: https://www.cdc.gov/infection-control/guidelines/index.html
For international patients, structured coordination helps reduce avoidable risk—verifying the provider, clarifying what’s included in fees, and ensuring a clear escalation pathway if anything deviates from normal healing.
The universal before‑care checklist for aesthetic procedures (what to do before treatment)
1) Verifying your provider and setting before any aesthetic procedure
Cosmetic treatments may look simple online, but safe practice requires deep anatomical knowledge and appropriate clinical standards. The American Academy of Dermatology (AAD) highlights that board‑certified dermatologists have the medical knowledge that can help lower complication risk.
External reference: https://www.aad.org/public/cosmetic/safety
Use this verification checklist:
- Confirm who performs the procedure (and their credentials/training).
- Ask whether the facility follows recognised infection control standards.
- Ask what happens if something goes wrong:
- Is there an emergency response protocol?
- Who do you contact after hours?
- Where would you be referred in an emergency?
- For injectables:
- Ask what product is used and how authenticity is ensured.
- Ask whether the clinic has a complication response plan (especially important for fillers).
If you’re researching clinics in Thailand, a directory with structured profiles can help you compare options systematically. Internal link: https://doodeena.com/
2) Medical screening and risk disclosure (bring more detail than you think you need)
A safe plan depends on full disclosure. Prepare a written list and share it in your consultation.
Tell your clinician about:
- Previous complications with procedures or anaesthesia
- Allergies (including adhesives/antiseptics)
- Tendency to form keloids or hypertrophic scars
- Autoimmune conditions or immune suppression
- Bleeding/clotting disorders
- Pregnancy or breastfeeding status
- History of cold sores (HSV), especially for perioral lasers/peels
Practical tip:
- Bring photos of any prior reactions or poor healing.
- List all prior fillers (type, location, approximate dates), if applicable.
3) Medications and supplements (avoid self‑adjusting prescriptions)
Some medicines and supplements can increase bruising or affect healing. Common examples include anticoagulants/antiplatelets, NSAIDs, and supplements such as high‑dose omega‑3 and vitamin E.
Key rule:
- Do not stop essential prescription medications unless the prescribing clinician specifically approves it.
4) “Prehab” lifestyle optimisation (especially before surgery)
Small changes can meaningfully affect recovery.
Focus on:
- Nicotine cessation (particularly important for surgery due to impaired wound healing)
- Consistent sleep and hydration
- Adequate protein intake
- Avoid scheduling too close to major events—bruising and swelling can be unpredictable
5) Skin preparation and sun management (device and peel patients—pay attention)
For laser‑based and peel‑based procedures, sun exposure is not a minor detail.
Before treatment:
- Avoid tanning and self‑tanner before laser hair removal and many laser treatments.
- Ask if your skin type or pigment history suggests a need for pre‑conditioning (clinician‑directed).
The universal aftercare framework for aesthetic procedures (what to do after treatment)
1) Skin barrier care and wound management after aesthetic procedures
A compromised skin barrier heals best with gentle support—not aggressive “active” skincare.
Core principles:
- Cleanse gently as instructed.
- Use only clinician‑recommended ointments/moisturisers.
- Do not pick scabs or force peeling.
- Delay retinoids, acids, and exfoliants until cleared.
2) Swelling and bruising management after aesthetic procedures
Most procedures involve some inflammation.
Common supportive steps (only if appropriate and clinician‑approved):
- Cold compresses for short periods
- Elevation (especially after facial procedures)
- Gentle early mobility when advised (particularly after surgery)
Expectation setting:
- Mild to moderate redness, swelling, and bruising can be normal.
- Worsening, disproportionate, or rapidly changing symptoms should be assessed promptly.
3) Photoprotection after aesthetic procedures (non‑negotiable for lasers, peels, microneedling)
Sun exposure after skin‑disrupting treatments increases risk of pigment problems, including PIH (higher risk in higher Fitzpatrick skin types).
After treatment:
- Prioritise physical sun avoidance (shade, hats).
- Use broad‑spectrum, high‑SPF sunscreen when permitted by your clinician.
4) Activity and exposure restrictions after aesthetic procedures
Many complications come from doing “normal life” too soon.
Common restrictions (follow your provider’s exact timeline):
- Avoid heat exposure (saunas, hot tubs)
- Avoid pools/open water until cleared
- Avoid strenuous exercise for the clinician‑specified window
- Follow sleep positioning instructions (e.g., head elevation after facial surgery)
5) Avoiding conflicting products and treatments after aesthetic procedures
Avoid stacking irritation.
Delay until cleared:
- Facials and facial massage
- Exfoliation and peels
- Additional energy‑based treatments
- Strong actives (retinoids, acids, high‑strength vitamin C)
6) Red‑flag symptoms after aesthetic procedures: when to seek urgent care
Call your clinic urgently—or seek emergency care—if you notice any of the following.
Infection (any procedure): fever, spreading redness, pus, worsening pain
Vascular compromise (fillers): severe pain, blanching, livedo/mottling, cool skin, ulceration
Vision symptoms (fillers): any change in vision = immediate emergency
Post‑surgical red flags: shortness of breath or chest pain (possible clot), rapidly expanding swelling, severe pain disproportionate to the procedure
Procedure playbooks: before and after care for popular aesthetic procedures (what to do, what to expect)
Botulinum toxin injections: before and after care
Who it’s for: Patients aiming to soften expression lines; outcomes vary by dose, anatomy, and technique.
Before care
- Disclose neuromuscular conditions and prior reactions.
- Share pregnancy/breastfeeding status.
- Discuss bruising risk if you take blood‑affecting medications/supplements.
Aftercare (first 24–48 hours)
- Stay upright for the period advised.
- Avoid rubbing or massaging treated areas.
- Avoid strenuous exercise, saunas, and alcohol for the advised window.
Typical timeline
- Onset in a few days
- Peak effect around 1–2 weeks
- Duration roughly 3–4 months (variable)
Common side effects vs red flags
- Expected: mild bruising, headache
- Needs review: drooping eyelid/brow, significant asymmetry, any systemic‑type symptoms
External reference (product safety): https://www.fda.gov/medical-devices/aesthetic-cosmetic-devices/botulinum-toxin-type-products-cosmetic-use
Dermal fillers (hyaluronic acid): before and after care
Who it’s for: Patients seeking volume/contour; product choice and technique matter.
Before care
- Disclose any prior fillers (type, area, timing).
- Discuss autoimmune history and any prior nodules or granulomas.
- If on anticoagulants, coordinate medication decisions with your prescribing clinician.
Aftercare (first 24–48 hours)
- Use clinician‑approved cold compresses if advised.
- Avoid heavy pressure, massage, or facial treatments for the specified period.
- Avoid high heat and heavy exertion initially if instructed.
Typical timeline
- Swelling often improves over days.
- “Settling” may take 1–2+ weeks, depending on product and area.
Common side effects vs red flags
- Expected: tenderness, swelling, bruising
- Emergency red flags: severe pain, blanching/mottling, coolness, ulceration, any vision change
Laser hair removal: before and after care
Who it’s for: Patients reducing hair growth over multiple sessions; settings should match skin type and hair characteristics.
Before care
- Avoid tanning/self‑tanner.
- Follow shaving protocol; avoid waxing/plucking beforehand.
- Review photosensitising medications if relevant.
Aftercare (first 24–48 hours)
- Gentle skincare; cool compresses for redness if advised.
- Avoid hot showers, saunas, and vigorous exercise briefly if instructed.
- Strict sun avoidance and sunscreen.
Typical timeline
- Multiple sessions required.
- Hair shedding can occur over 1–3 weeks.
Watch for
- Burns, blistering, pigment changes—seek assessment promptly.
Resurfacing lasers (non‑ablative vs ablative CO₂/Er:YAG): before and after care
Who it’s for: Patients targeting texture, scars, or photodamage; downtime varies widely.
Before care
- Screen for keloid history and PIH risk.
- Review isotretinoin history/timing.
- HSV prophylaxis may be recommended for some patients.
Aftercare (first week)
- Follow cleansing and occlusive care instructions precisely (especially ablative).
- Do not pick crusting.
- Strict photoprotection; delay actives until cleared.
Typical timeline
- Non‑ablative: days of redness
- Ablative: longer downtime; erythema can last weeks
Watch for
- Infection (including HSV), prolonged redness, pigment change, scarring (rare)
Chemical peels (superficial to deep): before and after care
Who it’s for: Patients targeting tone/texture; depth must match risk profile and goals.
Before care
- Assess PIH risk and HSV history.
- Review topical actives in use.
- Ask about pretreatment if pigment‑prone.
Aftercare
- Gentle cleansing and bland moisturiser/ointment.
- Do not force peeling.
- Strict sun avoidance and sunscreen.
Typical timeline
- Superficial: a few days of flaking
- Medium/deep: longer downtime, higher PIH risk
Watch for
- Burns, infection, scarring, pigment changes—seek timely review
Microneedling (with/without RF; with/without PRP): before and after care
Who it’s for: Patients targeting texture and mild scarring; outcomes build gradually.
Before care
- Avoid irritating actives immediately before (as instructed).
- Defer treatment if you have active infection or certain skin flares.
Aftercare (first 24–48 hours)
- Gentle skincare; avoid makeup for the clinician‑defined window (often ~24 hours).
- Avoid heat/excess sweating initially.
- Sun avoidance and sunscreen when cleared.
Typical timeline
- Redness usually 1–3 days
- Collagen changes develop over weeks
Watch for
- Infection, PIH, unusual track marks (rare)
Body contouring devices (cryolipolysis, RF, HIFU): before and after care
Who it’s for: Patients seeking gradual contour change; expectations should be realistic.
Before care
- Rule out contraindications (e.g., cold‑related disorders for cryolipolysis).
- Understand results are incremental, not immediate.
Aftercare
- Expect soreness, numbness, or bruising.
- Follow hydration and activity guidance.
Typical timeline
- Results over weeks to months
Watch for
- Persistent pain, unusual lumps; rare paradoxical adipose hyperplasia (cryolipolysis)
Liposuction (surgical): before and after care
Who it’s for: Selected surgical candidates; requires medical clearance and careful recovery planning.
Before care
- Medical clearance and VTE risk assessment.
- Nicotine cessation.
- Plan compression garments and at‑home support.
Aftercare (first week and beyond)
- Wear compression as instructed.
- Early ambulation as directed.
- Follow incision/drain care instructions.
Typical timeline
- Swelling and bruising: weeks
- Final contour: months
Red flags
- Fever, worsening redness, fluid collections
- Shortness of breath/chest pain (possible clot) = emergency
Rhinoplasty (surgical): before and after care
Who it’s for: Patients seeking structural/aesthetic nasal change; healing is long‑term.
Before care
- Stop nicotine.
- Review bleeding‑risk medications with your clinician.
- Plan adequate recovery time.
Aftercare
- Splint care; head elevation.
- Avoid nose blowing, heavy lifting, and trauma.
- Saline rinses if prescribed.
Typical timeline
- Bruising/swelling: 1–2+ weeks
- Refinement: many months
Watch for
- Bleeding, infection, breathing changes, significant asymmetry
Blepharoplasty (surgical): before and after care
Who it’s for: Patients addressing eyelid skin/fat changes; requires careful eye‑safety planning.
Before care
- Discuss dry eye history.
- Anticoagulant management must be coordinated with the prescribing clinician.
- Arrange assistance for the first days.
Aftercare
- Cold compresses early if advised.
- Head elevation; prescribed ointment/eye drops.
Red flags (urgent)
- Severe pain, vision change, rapidly expanding swelling—seek urgent assessment
Typical timeline
- Bruising/swelling: 1–2 weeks
Downtime planning for aesthetic procedures (how to build recovery into your travel schedule)
Downtime is not just time off work—it’s time for swelling to settle, skin to re‑epithelialise, and for you to be near appropriate follow‑up care.
Use these planning anchors:
| Procedure category | Typical downtime (general) | What to plan around |
|---|---|---|
| Injectables (botulinum toxin, fillers) | Hours to a few days | Bruising/swelling unpredictability; avoid major events |
| Energy‑based devices | Days (non‑ablative) to weeks (ablative) | Sun exposure, skin sensitivity, PIH risk |
| Surgery | Weeks to months (full maturation) | Follow‑ups, compression, mobility, clot‑risk precautions |
Practical planning checklist:
- Build a buffer window before weddings, filming, conferences, and long‑haul flights.
- Avoid scheduling peels/lasers right before beach holidays or high UV exposure.
- If travelling internationally, don’t compress timelines—ensure you have:
- A clear follow‑up plan
- Written instructions
- A local escalation pathway if needed
Common myths about aftercare for aesthetic procedures (corrected)
- “If I have downtime, something went wrong.”
Not necessarily. Redness, swelling, and bruising can be normal parts of healing. The key is knowing the difference between expected effects and red flags. - “Natural remedies are always safe on healing skin.”
Not always. Essential oils and unvetted actives can irritate healing skin and increase pigment risk. - “The more I cleanse and treat, the faster I heal.”
Over‑cleansing and early actives can prolong inflammation and increase PIH risk. - “A tan will hide redness after lasers or peels.”
Tanning after skin‑disruptive procedures can worsen pigment changes. Photoprotection is part of the treatment. - “All fillers can be dissolved if there’s a problem.”
Only hyaluronic acid fillers are reversible with hyaluronidase. This is an important informed‑consent point.